Why Choose DentalFirst?
At DentalFirst, we understand how challenging it can be to find a dentist who speaks your language. That’s why we’ve made it our mission to cater to individuals who prefer to communicate in English.
Our team of dental professionals consists of experienced dentists and dental hygienists who speak fluent English. We are committed to providing you with high-quality dental care while ensuring that you feel comfortable and at ease during your visit.


Comprehensive dental care tailored to your needs
DentalFirst offers a wide range of dental services, including preventive care, restorative dentistry, cosmetic dentistry, and emergency dental care.
Preventive Care
Our preventive care services include routine dental checkups, teeth cleaning, and fluoride treatment. We believe that prevention is the best approach to maintaining good oral health, and we’ll work with you to develop a personalized dental care plan that meets your needs.
Restorative Dentistry
If you’re experiencing dental problems such as cavities, gum disease, or tooth decay, we offer a variety of restorative dentistry services to help restore your smile. Our services include fillings, crowns, bridges, and dental implants.
Cosmetic Dentistry
Are you unhappy with the appearance of your teeth? At DentalFirst, we offer cosmetic dentistry services such as teeth whitening, veneers, and orthodontics to help you achieve a smile you can be proud of.
Emergency Dental Care
Cutting-Edge Technology, Convenient Location & Flexible Payment Options
Our Technology
At DentalFirst, we use state-of-the-art technology to ensure that our patients receive the best possible care. Our dental clinic is equipped with digital X-ray machines, intraoral cameras, and other advanced tools that allow us to diagnose and treat dental problems more accurately and efficiently.
Our Location
Conveniently located in Berlin Charlottenburg in the borough of Westend, DentalFirst is easily accessible by car or public transportation. Our office is equipped with comfortable chairs, air conditioning and air cleaning, and other amenities to help you feel relaxed and comfortable during your visit.
Our Payment Options
We understand that dental care can be expensive, which is why we offer a variety of payment options to make dental treatment more affordable. We accept most insurance plans, and we also offer financing options to help you spread the cost of treatment over time.
Advanced Treatments for a Healthy & Beautiful Smile
Comprehensive Dental Aesthetics

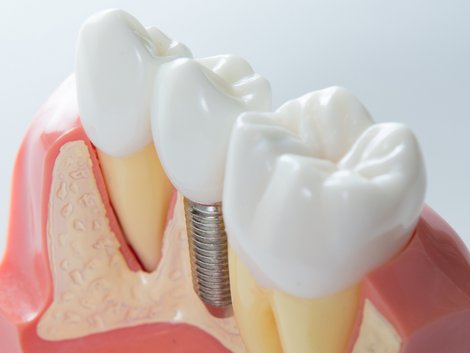
Dental Implants
Dental implants are artificial tooth roots that are firmly screwed to the jaw. They replace the natural tooth root after tooth loss. Dental prostheses from crowns to full dentures can then be fixed on these implants.

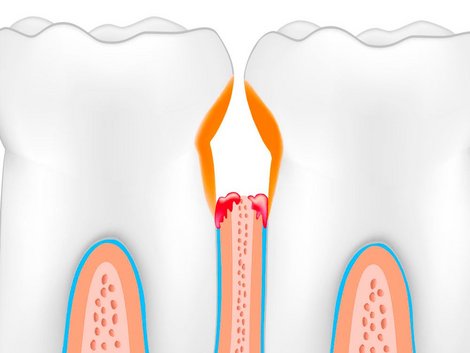
Periodontal (gum) disease
Periodontitis is a common reason for tooth loss. The inflammation in the periodontium usually proceeds painlessly at first and spreads gradually. It is often only noticed when the periodontal tissue is already severely affected. Clear indications of progressive periodontitis are bleeding, redness, swelling and regression of the gums.

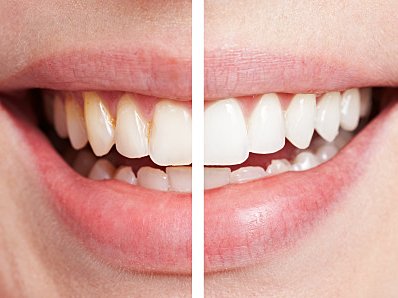
Teeth whitening
Are you unhappy with the color of your teeth? Do you avoid smiling in public due to embarrassment? Teeth whitening might be the solution you’re looking for! If you’re looking for a safe and effective teeth whitening treatment in Berlin, look no further than DentalFirst Berlin.

Fear of the Dentist / Dentophobia
Dentophobia – or fear of dentists – is a common phobia among people of all ages. Due to unpleasant or painful experiences in the past, some patients fear going to the dentist so much that their teeth deteriorate over time without getting treatment. This causes additional pain and shame and even more fear of making the important appointment with the dentist.
We are here to help. Our practice has special treatments for patients with fear. We are helping you step by step to overcome possible fear or shame. If neccessary we can even provide General anaesthesia (narcosis) so you can undergo even big treatments.

Professional dental cleaning / prophylaxis
Professional tooth cleaning reduces the risk of tooth loss. Professional tooth cleaning is therefore not only a hygienic measure to remove tartar and plaque, but also an aesthetic treatment to remove discolouration. It contributes to your general health and well-being.

Craniomandibular dysfunction
Craniomandibular dysfunction refers to a disruption in the interaction between the chewing muscles, temporomandibular joint and teeth, often with a stressful effect on the entire body. In our practice (CMD competence centre) we treat acute and chronic temporomandibular joint complaints. The aim of treatment is to restore pain-free functioning of the chewing apparatus.

Lumineers / Veneers
Get in Touch
DentalFirst
Dental Practice Berlin
Reichsstraße 2 | 14052 Berlin | Charlottenburg-Wilmersdorf
Phone 030 – 308 20 996
Fax 030 – 302 98 33
Email rezeption@dentalfirst.de
For questions and appointment requests, please contact us by phone or write a message to rezeption@dentalfirst.de.
Sie sehen gerade einen Platzhalterinhalt von Google Maps. Um auf den eigentlichen Inhalt zuzugreifen, klicken Sie auf die Schaltfläche unten. Bitte beachten Sie, dass dabei Daten an Drittanbieter weitergegeben werden.
Mehr InformationenBook Your Appointment Today
Confirmation of Appointment
Please note, that an appointment needs to be confirmed by the practice. Our english speaking staff will contact you as soon as possible by email or telephone to confirm or offer an alternative date. If anything prevents you from keeping an appointment, we kindly request you to cancel within 24 hours in advance.